
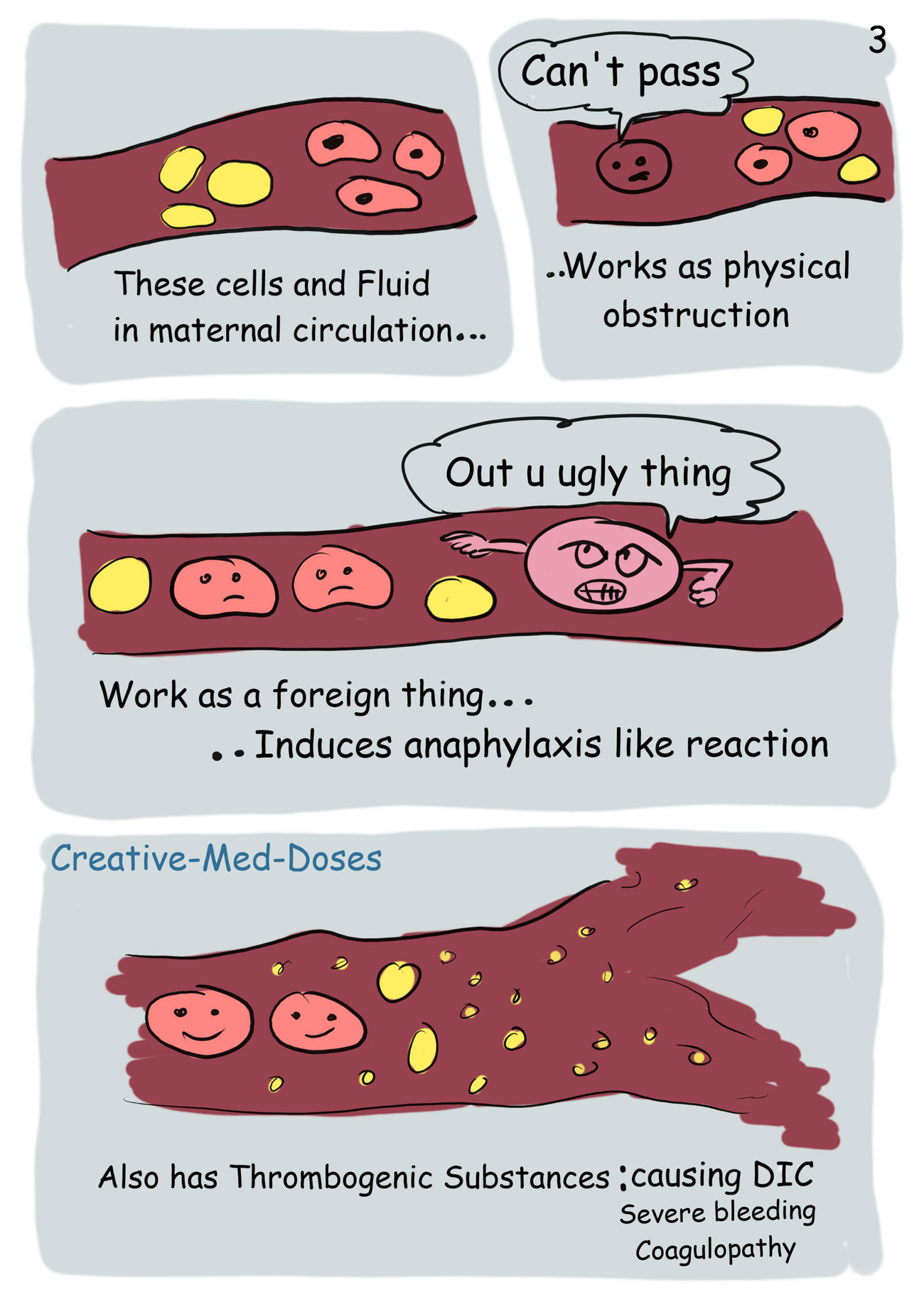
The traditional treatment is supportive and aimed at treating cardiovascular, pulmonary, and coagulation derangements. Prompt recognition of the symptoms and immediate interdisciplinary management are pivotal for prognosis. In fact, several diagnostic biomarkers have been proposed, but they have not been established in routine clinical diagnosis. Thus, the diagnosis is one of exclusion, very often on post-mortem report. In severe cases, AFE should be distinguished from other acute and life-threatening emergencies, such as pulmonary embolism, myocardial infarction and peripartal cardiomyopathy. There is great variability in the presentation of AFE from classical cardiopulmonary collapse with coagulopathy to minor and subclinical presentations. Even though there is no shared pathogenetic theory for AFE, the transfer of amniotic fluid components in the maternal circulation may lead either to an inflammatory-mediated anaphylactoid response or to complement activation.

Furthermore, persistent neurological impairment has been reported in 6-61% of survivors. With a mortality of 0.5 to 1.7 deaths per 100,000 deliveries in the developed world and 1.9 to 5.9 deaths per 100,000 deliveries in the developing world, it is among the leading direct causes of maternal death.
AFE is a rare and life-threatening obstetric condition, occurring in 2 to 8 per 100 000 births. This article reviews the current evidence on amniotic fluid embolism (AFE), focusing on epidemiology, pathogenesis, clinical presentation, diagnosis and treatment.


 0 kommentar(er)
0 kommentar(er)
